Un-Pinch the Nerve. Avoid the Scalpel. Keep Your Hands Working.
Waking up at 3:00 AM with numb, burning hands is exhausting. Being told you need surgery is terrifying. We utilize advanced Ultrasound-Guided Hydrodissection—a 'liquid scalpel' that gently washes away scar tissue to instantly free trapped nerves with zero surgical incisions and zero downtime.
Message Us to Book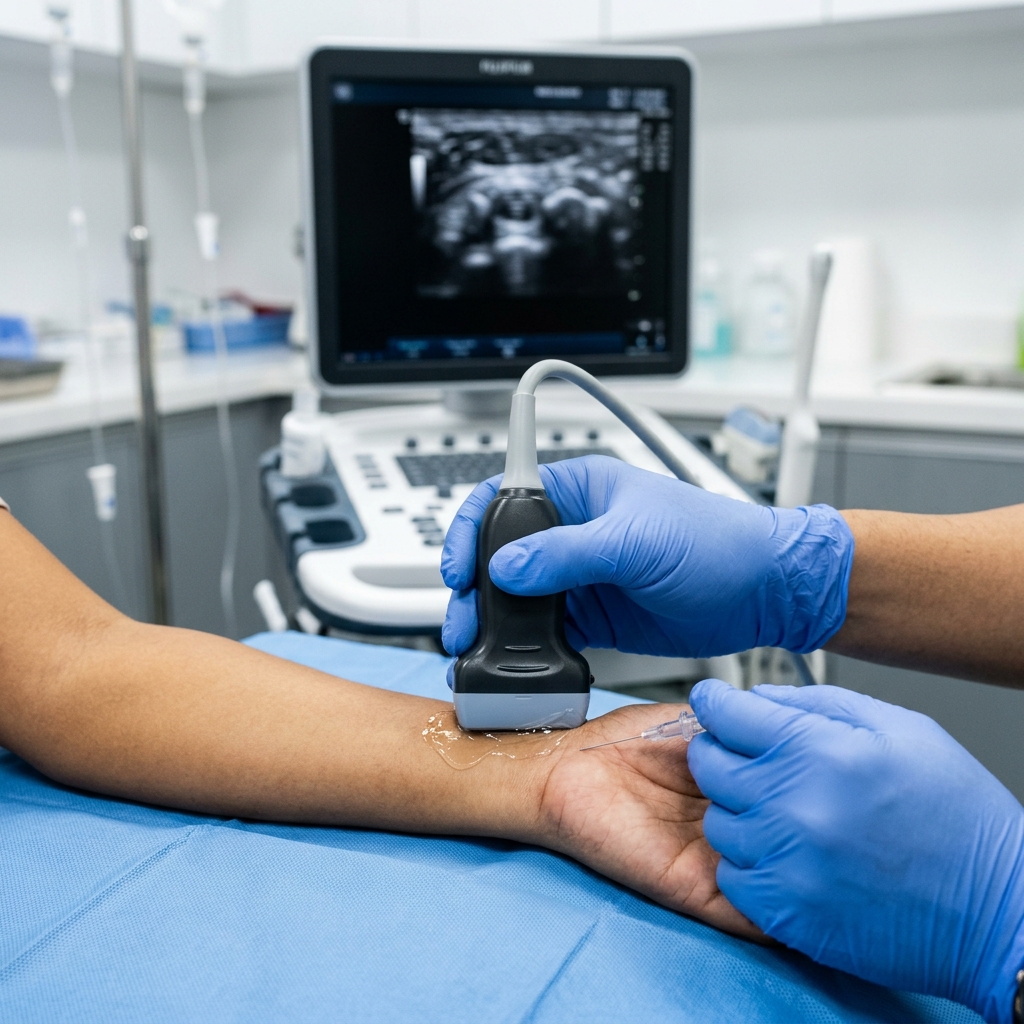
The 'Liquid Scalpel' for Trapped Nerves
If you are suffering from Carpal Tunnel Syndrome or a pinched nerve in your arm or leg, you already know the frustration. You drop coffee cups because your grip strength is failing. You violently shake your hands in the middle of the night trying to get the feeling back. Eventually, a doctor may look at you and say, 'We need to cut your wrist open to release the pressure.' For a professional, a manual laborer, or a parent, taking 4 to 6 weeks off work to recover from surgery is financially and physically devastating.
At TeraCare, we offer a state-of-the-art alternative: Ultrasound-Guided Nerve Hydrodissection. Instead of using a steel scalpel to slice through your ligaments, we use a 'Liquid Scalpel.' Dr. Rabara uses high-definition ultrasound to locate the exact millimeter where the nerve is crushed by sticky scar tissue. We then inject a precise stream of healing fluid directly around the nerve. This fluid gently peels the scar tissue away and creates a protective fluid cushion, instantly un-pinching the nerve without a single stitch.
Pinched Nerves We Un-Tether
Is Hydrodissection Right For You?
Stopping the Damage Before It's Permanent
Nerves are fragile. If they are crushed for too long, the numbness becomes permanent, and the muscles begin to waste away. Hydrodissection is the ultimate bridge between taking useless pain pills and undergoing invasive surgery.
You are an EXCELLENT candidate if:
- You wake up with numb, tingling, or "asleep" hands and feet.
- You have been diagnosed with Carpal Tunnel Syndrome but absolutely cannot afford the downtime of surgery.
- You experience sharp, electric pain that shoots down your arm or leg when you move a certain way.
- You have tried wrist splints, rest, and generic anti-inflammatory pills with zero success.
You may NOT be a candidate if:
- You have waited so long that the muscles in your hand or leg have completely hollowed out (severe atrophy), indicating the nerve may be permanently dead.
- You have a massive structural cyst or a bone spur physically cutting into the nerve, which physically requires a surgeon to remove.
The Realities of the Procedure
Hydrodissection is a highly advanced, ultra-precise medical technique. While it avoids the risks of open surgery, we believe in complete transparency regarding the procedure:
- Temporary Numbness & Heaviness: We inject a large volume of fluid (including a mild anesthetic) directly around the nerve. Your hand or leg will feel heavy, thick, and completely numb for roughly 2 to 6 hours after the procedure.
- It is a Structural Fix, Not Magic: We are using fluid to stretch the tissue. You may feel a sensation of tightness or pressure during the injection. It may take several days for the swelling to subside and the nerve to "breathe" again before you feel the maximum relief.
- Multiple Sessions May Be Needed: For mild nerve entrapment, a single session can provide a permanent cure. For severe, chronic scar tissue that has been building up for years, a series of 2 to 3 hydrodissection sessions spaced several weeks apart may be necessary to fully peel the nerve free.
Why the "Liquid Scalpel" is the Superior Choice
A surgeon cuts open your skin and slices through the ligament pressing on the nerve. Requires stitches, casting, and 4 to 6 weeks of downtime. High risk of new scar tissue.
Dr. Rabara uses an ultrasound screen to guide the needle exactly next to the nerve, using a gentle wave of fluid to wash away the scar tissue. Zero surgical cuts.
A doctor injects a steroid into your wrist based on "feeling" the anatomy. High risk of nerve damage if the needle hits the nerve. Steroids only hide swelling.
Your Rapid Return to Normalcy
The Numbness Phase
Your limb will feel wonderfully pain-free, but heavily numb. Protect the limb during this window until normal sensation returns.
The Healing Phase
The body slowly absorbs the therapeutic fluid cushion. Nighttime numbness should already be massively reduced or completely gone.
Prevention
We prescribe specific nerve-gliding exercises and Occupational Therapy ergonomics to ensure the scar tissue never returns.
Clinical Science & Technical Details
For our medical colleagues and highly analytical patients, we provide these transparent technical details on the pathophysiology and interventional protocols.
Explore the Clinical Science: Perineural Fibrosis and Ischemic Compression
The pathophysiology of peripheral nerve entrapment is fundamentally a mechanical issue leading to localized ischemia. When a nerve passes through a narrow fibrosseous tunnel, repetitive micro-trauma causes the surrounding fascia to thicken. This perineural fibrosis adheres directly to the nerve's epineurium, restricting its natural glide.
Hydrodissection mechanically reverses this ischemia. By utilizing high-resolution ultrasound to visualize the fascial planes, an anechoic fluid (typically a mixture of normal saline, 5% Dextrose, and local anesthetic) is injected precisely under high pressure. This fluid acts as a hydraulic wedge, physically dissecting the constricting fibrotic tissue away from the epineurium, instantly restoring the intraneural microcirculation.
Detailed Diagnostic Pathways: Cross-Sectional Area (CSA) Measurement
At our Vigan City clinic, patient selection for Hydrodissection is fiercely data-driven. Dr. Rabara utilizes Diagnostic MSK Ultrasound to objectively quantify the degree of nerve compression before any intervention occurs.
For Carpal Tunnel Syndrome, we measure the Cross-Sectional Area (CSA) of the median nerve. A normal median nerve typically measures between 6 to 9 mm². In severe entrapment, the nerve swells proximal to the compression site (the 'notch sign'), often measuring well over 12 mm² to 15 mm². Calculating this ratio allows us to confirm structural integrity and determine if the nerve possesses enough health to respond to hydrodissection.
Advanced Systemic Screening and EMG/NCV Correlation
While hydrodissection is remarkably safe, determining its clinical appropriateness requires correlating sonographic findings with electrodiagnostic studies. Dr. Rabara frequently reviews the patient's Electromyography and Nerve Conduction Velocity (EMG/NCV) reports.
If an EMG reveals profound axonal loss with active denervation potentials in the target muscle, it indicates end-stage entrapment where hydrodissection may only provide temporary relief. We transparently educate these patients when surgical release is the definitive necessity to prevent total loss of function.
Pharmacokinetics of 5% Dextrose (D5W) and TRPV1 Downregulation
While normal saline and local anesthetics provide excellent mechanical separation, TeraCare frequently utilizes 5% Dextrose in Water (D5W) as the primary dissecting fluid. This approach is deeply rooted in Perineural Injection Therapy (PIT) principles.
Recent neurophysiological research indicates that chronic nerve entrapment causes an upregulation of Transient Receptor Potential Vanilloid 1 (TRPV1) cation channels, responsible for severe burning pain. Dextrose acts directly on these receptors, instantly downregulating them and stopping the release of pro-inflammatory neuropeptides like Substance P. This provides both hydraulic release and a natural neuromodulatory effect.
Inside the Procedure: In-Plane Needle Tracking and the Anechoic Halo
The clinical safety of Hydrodissection relies entirely on the operator's proficiency with high-frequency linear ultrasound transducers. Dr. Rabara utilizes a strict in-plane needle approach, meaning the entire shaft and tip of the needle are clearly visualized on the monitor at all times.
As the D5W fluid is injected, it appears black (anechoic) on the ultrasound screen. Dr. Rabara carefully manipulates the needle to ensure this fluid completely encompasses the nerve 360 degrees, creating the classic 'anechoic halo' sign. This visual confirmation guarantees that the nerve has been completely liberated from all sides without ever piercing the nerve bundle itself.
Axonal Transport Restoration and Remyelination
The biological timeline for complete nerve healing extends beyond the immediate mechanical release. Chronic compression disrupts the axoplasmic flow (the internal transport system of the nerve cell), leading to Wallerian degeneration in severe cases.
Once Hydrodissection restores the microvascular blood supply, the nerve begins the slow process of biological repair. Remyelination occurs over the course of several weeks to months. During this period, the patient will notice steady improvemen in grip strength and cessation of nocturnal paresthesias.
Seeing is Believing: The Procedure
The MSK Ultrasound Mapping
Nerves are tiny—often the size of a spaghetti noodle. Dr. Rabara places the ultrasound probe on your skin to locate the exact millimeter where the nerve is crushed.
The Liquid Release
While watching the monitor, Dr. Rabara guides a microscopic needle directly next to the nerve and injects a specialized healing fluid to peel away scar tissue.
Immediate Mobility
The procedure takes less than 20 minutes. Because no incisions were made, you can walk out of the clinic and return to work the very next day.
Common Questions
Does the hydrodissection procedure hurt?
The procedure is highly tolerable. We use an ultra-fine needle and apply local anesthetic to completely numb the skin and the tissue pathway before we begin. You will feel a sensation of "fullness" or pressure as the fluid expands around the nerve.
Will I need to wear a cast or splint afterward?
No! That is the greatest advantage of avoiding surgery. There are no stitches and no casts. We encourage you to move your hand or leg normally after the numbness wears off help the nerve glide freely.
How much does Hydrodissection cost compared to surgery?
Hydrodissection is significantly more cost-effective than open release surgery. It eliminates the costs of an operating room, an anesthesiologist, and weeks of lost income.
Is Ultrasound-Guided Hydrodissection covered by PhilHealth or my HMO?
Yes, because this is an advanced, medically necessary interventional procedure to treat documented nerve entrapment, it is frequently eligible for coverage. Our clinic administration will assist you with necessary documentation.
I have had Carpal Tunnel for 5 years. Is it too late for this to work?
It depends on the level of muscle damage. If you have thumb muscle strength remaining, hydrodissection can absolutely work. Dr. Rabara will use ultrasound to evaluate the health of your nerve before we proceed.