Relieve the Pressure. Drain the Fluid. Restore the Joint.
When your knee or elbow suddenly swells like a balloon, the pain isn't just an ache—it is agonizing mechanical pressure. We use precision ultrasound to safely open the pressure valve, draining the trapped fluid for instant, profound relief.
Message Us to Book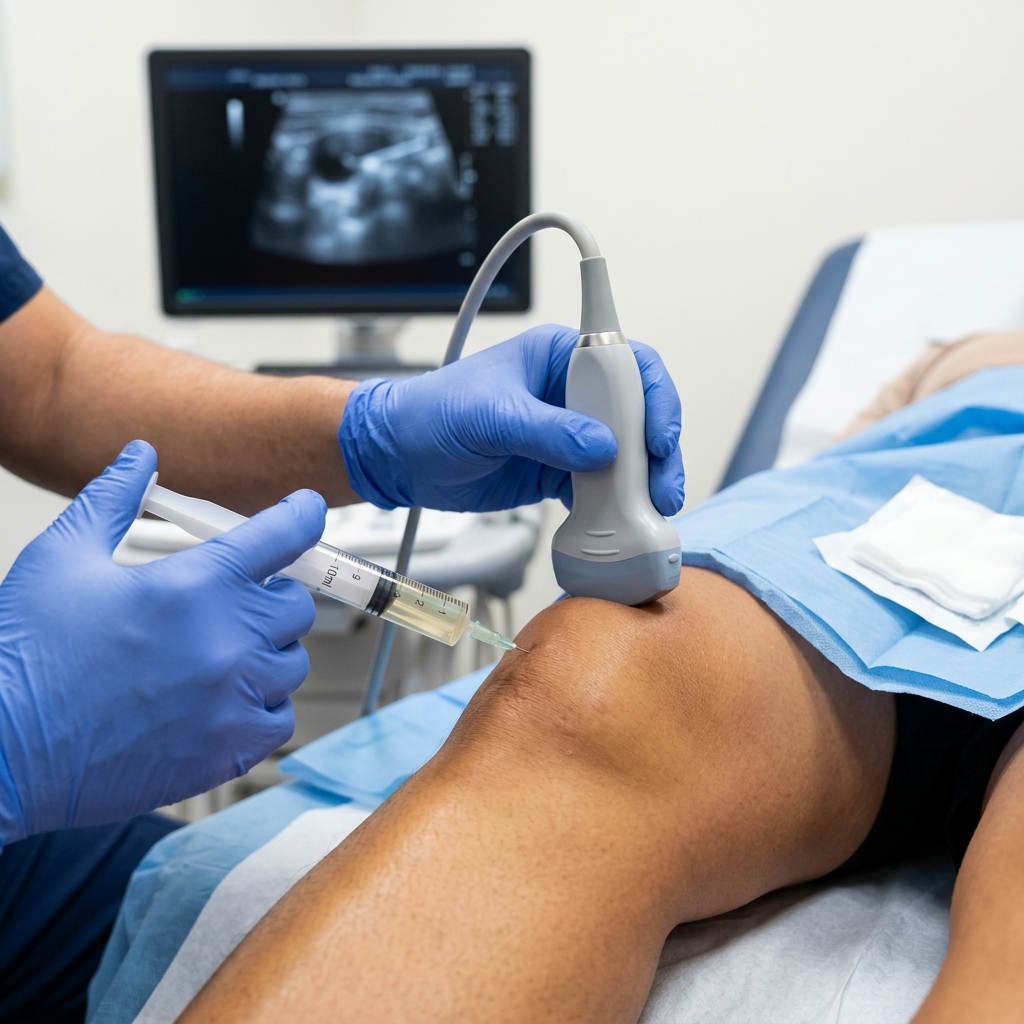
Opening the Pressure Valve
Seeing your joint swell to twice its normal size is terrifying. Whether it is "water on the knee," a massive Baker's Cyst, or a sudden Gout flare-up, the sensation is unmistakable: your joint feels incredibly tight, hot, and heavy. You literally cannot bend your leg or arm past a certain point because the trapped fluid is acting like a physical wall. The throbbing pain you feel is hydraulic pressure stretching the sensitive joint capsule to its absolute limit. Attempting to fix this at home with ice packs, elevation, or over-the-counter pain pills is useless.
To stop the pain, the fluid must be physically removed. Therapeutic Arthrocentesis (joint aspiration) is the medical equivalent of opening a pressure valve. Dr. Rabara utilizes live diagnostic ultrasound to pinpoint the exact deepest pocket of fluid. We guide a small needle safely into the joint and gently suction the fluid out. The moment the fluid is extracted, the mechanical pressure drops to zero, and the ability to bend your joint is instantly restored.
Joint Swelling We Actively Drain
Do You Need Your Joint Drained Today?
Recognizing the Hydraulic Crisis
An acute effusion is not a subtle injury. It is a physical, visible crisis that severely limits your mobility and demands immediate medical attention.
You are an EXCELLENT candidate if:
- Knee, elbow, or ankle is visibly swollen to nearly twice its normal size.
- Tight, throbbing pressure that gets worse when you try to bend the joint.
- Massive, tight bulge behind your knee (Baker's Cyst) that makes straightening leg impossible.
- Diagnosed history of Gout and experiencing a sudden, blindingly painful attack.
You may NOT be a candidate if:
- Severe, active skin infection (cellulitis) directly over the injection site.
- Open, draining wound that could push bacteria into the joint space.
The Realities of Joint Draining
We understand the fear of having a needle inserted into an already agonizing joint. We want you completely prepared for the "Drain and Treat" process:
- The "Two-Step" Protocol: Immediately after draining the fluid, we use the same needle to inject specialized medication to shrink the joint lining and "seal" the leak.
- Immediate Relief, Temporary Weakness: The joint capsule has been stretched like an old rubber band. You must wear a compression wrap and rest for a few days to allow tissue to tighten back up.
- Minimal Discomfort: We use powerful local anesthetic. Because we use ultrasound guidance, we go straight into the empty pocket without painfully scraping bone or cartilage.
Why You Cannot Drain a Joint "Blindly"
Applying ice and waiting for swelling to go down on its own. Inflammatory fluid acts like acid, destroying healthy cartilage if left to sit.
Dr. Rabara sees the exact size, depth, and location of the fluid pocket on screen. Guaranteed 100% empty and accurate medicine delivery.
A doctor feels the outside of the joint and pokes based on landmarks. Frequently hits bone or misses deep pockets entirely.
What Happens After the Fluid is Gone?
The Compression Phase
You must wear a tight compression bandage (Ace wrap). This physically prevents the empty joint space from filling back up while medication works.
The Calming Phase
Anti-inflammatory medication takes full effect, shutting down the 'fire' inside. The joint may feel 'loose' as ligaments were stretched by swelling.
Addressing the Root Cause
We investigate the cause (meniscus tear, gout, arthritis) and prescribe Physical Therapy to ensure the swelling never returns.
Clinical Science & Technical Details
For our medical colleagues and highly analytical patients, we provide these transparent technical details on the pathophysiology and interventional protocols.
Explore the Clinical Science: Synovial Capsular Distension and Inflammatory Exudate
Normal synovial fluid is small in volume. During an acute inflammatory cascade, the synovial membrane dramatically increases vascular permeability, flooding the joint cavity with low-viscosity exudate rich in pro-inflammatory cytokines and degradative enzymes.
Rapid accumulation causes severe capsular distension, creating excruciating ischemic and mechanical pain. Evacuating this fluid is critical; if left to sit, degradative enzymes will actively destroy healthy articular cartilage.
Detailed Diagnostic Pathways: Synovial Fluid Analysis & Septic Arthritis
A clear, yellowish fluid typically indicates non-inflammatory osteoarthritis. Cloudy, watery fluid indicates a severe inflammatory process like Gout or Pseudogout.
Crucially, grossly purulent fluid suggests Septic Arthritis (bacterial infection). This is an absolute orthopedic emergency, and diagnostic aspiration allows for immediate fluid culture.
Advanced Systemic Screening and Baker's Cyst Rupture
For posterior knee swelling, Dr. Rabara must differentiate between a ruptured Baker's Cyst and Deep Vein Thrombosis (DVT) using diagnostic ultrasound.
If a cyst is intact but causing severe mechanical block, we perform ultrasound-guided aspiration frequently followed by fenestration of the cyst wall to prevent immediately re-accumulation.
Preventing Iatrogenic Infection and Rebound Effusions
While rare, Dr. Rabara utilizes rigorous aseptic technique. The skin is aggressively prepped with Chlorhexidine, and sterile ultrasound probe covers are mandated.
To prevent 'rebound effusion', we introduce a highly localized, long-acting corticosteroid into the newly evacuated space, suppressing the vascular permeability that caused the exudate.
Inside the Procedure: Suprapatellar Pouch Navigation and Dynamic Compression
Using a lateral approach with a linear transducer, Dr. Rabara visualizes the anechoic fluid collection in the suprapatellar recess, superior to the patella and deep to the quad tendon.
To ensure 100% evacuation, we apply dynamic manual compression ('milking') to the medial and lateral gutters, forcing loculated fluid into the suprapatellar pouch for extraction.
Restoring Capsular Integrity and Proprioceptive Function
A massive joint effusion causes Arthrogenic Muscle Inhibition (AMI)—a reflexive neurological shut-down of the VMO muscle to protect the joint.
Post-aspiration rehab is not optional. Dr. Rabara refers patients to our therapy team to re-establish neuromuscular control and proprioceptive balance training.
The Joint Drain and Treat Protocol
The Ultrasound Target Mapping
Dr. Rabara uses high-resolution ultrasound to map a needle trajectory that completely avoids your bones, cartilage, and major blood vessels.
The Pressure Release
After numbing the skin, we gently suction the inflammatory fluid while watching the screen. You will feel agonizing, tight pressure disappear in seconds.
The "Sealant" Injection
We leave the needle in place and inject targeted medication (Steroid or Gel). This calms the joint lining, ensuring the swelling does not return tomorrow.
Common Questions
Does draining the fluid hurt?
The anticipation is almost always worse than the procedure itself. We aggressively numb the skin and tissue with a local anesthetic before the drainage needle ever enters. Because we use ultrasound, there is no painful "digging" around.
Will the fluid just come right back?
If a doctor ONLY drains the fluid, it often comes back. This is why Dr. Rabara strictly utilizes the "Drain and Treat" protocol, immediately injecting medication to shut down the cells producing the fluid.
How much fluid is typically drained from a knee?
A normal knee has less than 5ml. During a severe acute effusion, Dr. Rabara routinely extracts anywhere from 30cc to over 100cc (about half a cup) of trapped inflammatory fluid.
Is joint aspiration covered by PhilHealth or my HMO?
Yes, Therapeutic Arthrocentesis is a standard, medically necessary orthopedic intervention. It is frequently eligible for coverage under many major HMO packages and PhilHealth.
Can I walk out of the clinic after getting my knee drained?
Yes, absolutely. You will likely walk better because the mechanical block is gone. However, we ask that you rest and elevate the leg for 48 hours to protect the joint capsule.