Promote Natural Healing and Help Delay Surgery with Regenerative Medicine.
Platelet-Rich Plasma (PRP) and Prolotherapy offer a premium, evidence-based approach to managing chronic joint pain, supporting tissue recovery, and restoring your mobility without relying on invasive joint replacement.
Message Us to Book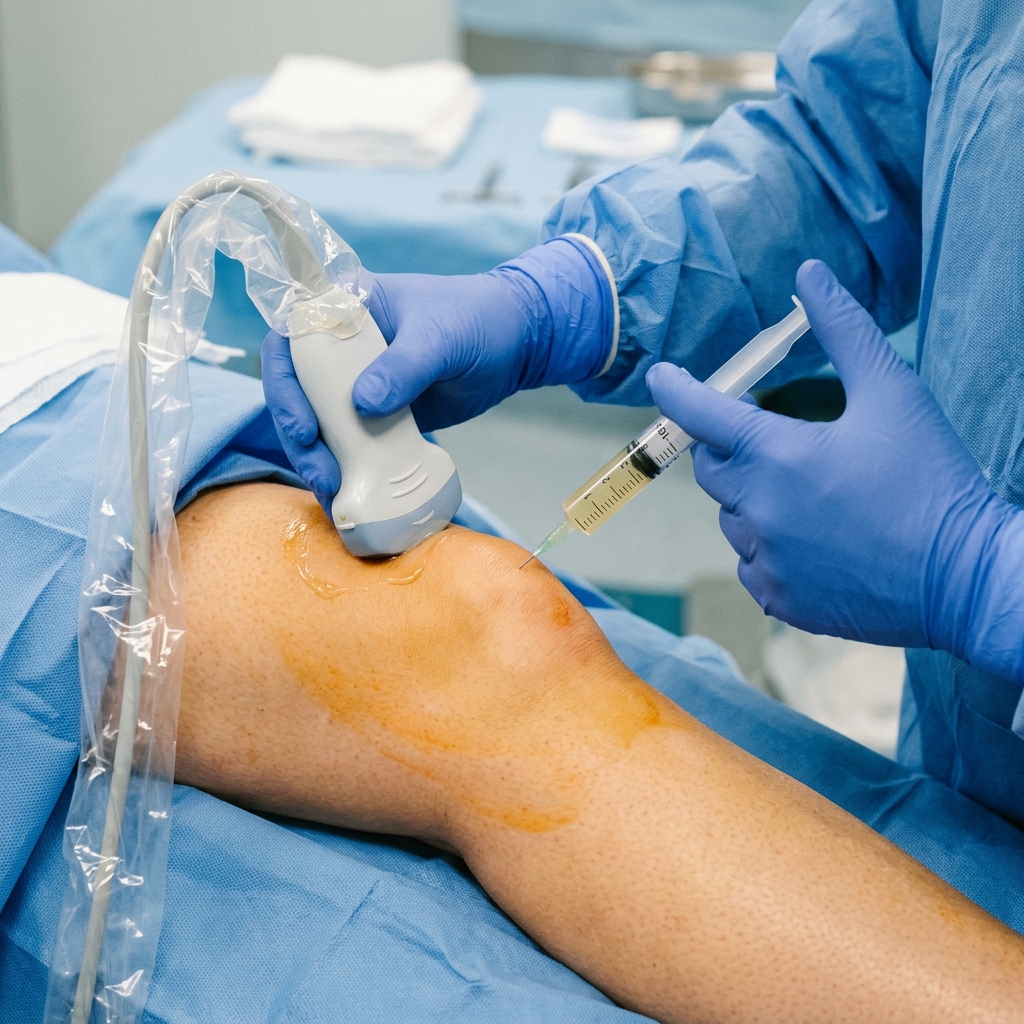
What is Platelet-Rich Plasma (PRP) Therapy?
For decades, the standard medical approach to chronic joint pain has been masking the symptoms with oral medications or applying temporary patches with corticosteroid injections. Regenerative Medicine represents a fundamental shift in physiatry. Instead of merely suppressing the pain, PRP therapy actively utilizes the healing properties inherent in your own body to address the structural root cause of your discomfort.
Your blood contains platelets, which are packed with specialized proteins called 'growth factors.' When you sustain an injury, your body naturally rushes these platelets to the site to initiate repair. PRP therapy takes this natural biological process and amplifies it. By drawing a small sample of your blood, concentrating these platelets in a centrifuge, and precisely re-injecting them into your damaged joint or tendon, we deliver a powerful, concentrated dose of healing factors exactly where your body needs it most.
What Conditions Can Regenerative Medicine Treat?
Is a Guided PRP Injection Right for You?
Regenerative medicine is highly effective, but it is not a universal cure. During your comprehensive consultation, Dr. Rabara will conduct a thorough musculoskeletal evaluation to determine if your specific condition will respond to orthobiologic treatments.
You are an EXCELLENT candidate if:
- Chronic tendon, ligament, or joint pain that has not responded to rest or PT.
- Seeking to delay or avoid invasive orthopedic surgery.
- Desire to reduce reliance on pain meds or repeated steroid injections.
You may NOT be a candidate if:
- Complete 'bone-on-bone' advanced osteoarthritis.
- Active systemic infections, blood disorders, or malignancies.
- Currently taking high doses of blood thinners or systemic steroids.
Understanding the Risks and Realities of PRP
As a PMA-accredited clinic, we believe in complete clinical transparency. Because PRP utilizes your own blood (an autologous treatment), the risk of allergic reaction, rejection, or disease transmission is exceptionally rare. However, as with any injection-based medical procedure, there are clinical realities you must consider:
- Post-Injection Flare: It is common to experience a temporary increase in localized pain, swelling, and stiffness for 3 to 7 days following the procedure. This is a normal biological response.
- No Guaranteed Outcomes: While clinical studies show high success rates, individual physiological responses vary. We cannot legally guarantee a 100% resolution of symptoms.
- Infection & Bleeding: Though we adhere to strict, sterile clinical protocols, any injection carries a minimal risk of localized infection or minor bleeding.
- Multiple Sessions: Depending on the severity of your tissue damage, a single injection may not be sufficient. Some patients require a targeted series of 2 to 3 injections.
How Does PRP Compare to Traditional Treatments?
Suppresses inflammation temporarily. Relief lasts weeks to a few months.
Stimulates biological tissue repair and cellular growth. Long-lasting functional improvement.
Removes the biological joint and inserts artificial components.
What to Expect After Your Procedure
The Inflammatory Phase
You may experience localized soreness and swelling as the growth factors initiate the healing process.
The Proliferation Phase
Soreness subsides. You will begin structured, gentle physical therapy to support new tissue formation.
The Remodeling Phase
Expect progressive improvements in joint mobility and measurable reductions in chronic discomfort.
Clinical Deep-Dive: The Science of PRP
Advanced orthobiologic insights into how your own blood heals damaged joints.
The Biology of Platelet-Rich Plasma
The therapeutic potential of PRP lies within the alpha-granules of your platelets. When these platelets are concentrated and subsequently activated at the site of injury, they release a potent cocktail of bioactive signaling proteins.
This includes PDGF (Platelet-Derived Growth Factor) for cell replication, VEGF for angiogenesis, and TGF-beta1 for collagen production. By concentrating these factors up to 5-10 times their baseline levels, we provide a massive biological stimulus to tissues like tendons and ligaments that naturally have poor blood supply.
Advanced Indications: Tendinopathy vs. Osteoarthritis
Biologically, a 'tendinopathy' (like Plantar Fasciitis) is often a state of stalled healing. PRP restarts this clock by introducing fresh PDGF and VEGF to stimulate fibroblast activity.
In the joint, PRP acts as a powerful modulator, shifting the environment from breakdown (catabolism) to repair (homeostasis). While PRP cannot usually 'regrow' lost joint space in advanced stages, it is highly effective in mild-to-moderate stages (Kellgren-Lawrence Grade 1-3) for reducing pain and delaying joint replacement surgery.
The 3-Step Clinical Process
Comprehensive Joint Evaluation
We conduct a thorough clinical and ultrasound assessment to confirm your diagnosis and ensure PRP is the appropriate clinical pathway.
Blood Draw & Centrifuge Processing
We safely draw a small volume of your blood and process it in a specialized medical centrifuge to isolate the platelet-rich plasma.
Ultrasound-Guided Precision Delivery
Utilizing high-resolution ultrasound imaging, Dr. Rabara precisely guides the concentrated PRP directly into the damaged structural tissue, ensuring maximum clinical efficacy.
Common Questions
How long does the PRP procedure take?
The entire outpatient procedure, from the initial blood draw to the final targeted injection and post-procedure observation, typically takes under one hour right here in our Vigan City clinic.
Is the injection painful?
Patient comfort is paramount. While some pressure is normal, we utilize local anesthetics and highly precise ultrasound guidance to ensure the clinical process is as tolerable and efficient as possible.
Is PRP covered by PhilHealth or my HMO?
Currently, Regenerative Medicine procedures like PRP and Prolotherapy are considered premium, elective treatments and are generally not covered by PhilHealth or standard HMOs. We provide a transparent, upfront cash-pay estimate prior to any treatment.
Can I drive myself home after the injection?
Most patients can drive themselves home if the injection was in an upper extremity. However, if you receive a PRP injection in your knee, ankle, or hip, we highly recommend arranging for someone to drive you home for safety and comfort.
Do I need physical therapy after my PRP injection?
Yes. Regenerative medicine is most effective when paired with a structured rehabilitation protocol. We will design a customized physical therapy plan to help you safely rebuild biomechanical strength as the joint heals.