Stop Guessing. Map the Exact Source of Your Nerve Pain.
Don't let numbness, tingling, or radiating pain go undiagnosed. Our precision Electromyography and Nerve Conduction Velocity (EMG-NCV) testing provides the exact, objective data needed to map your nerve health and build a targeted recovery plan.
Message Us to Book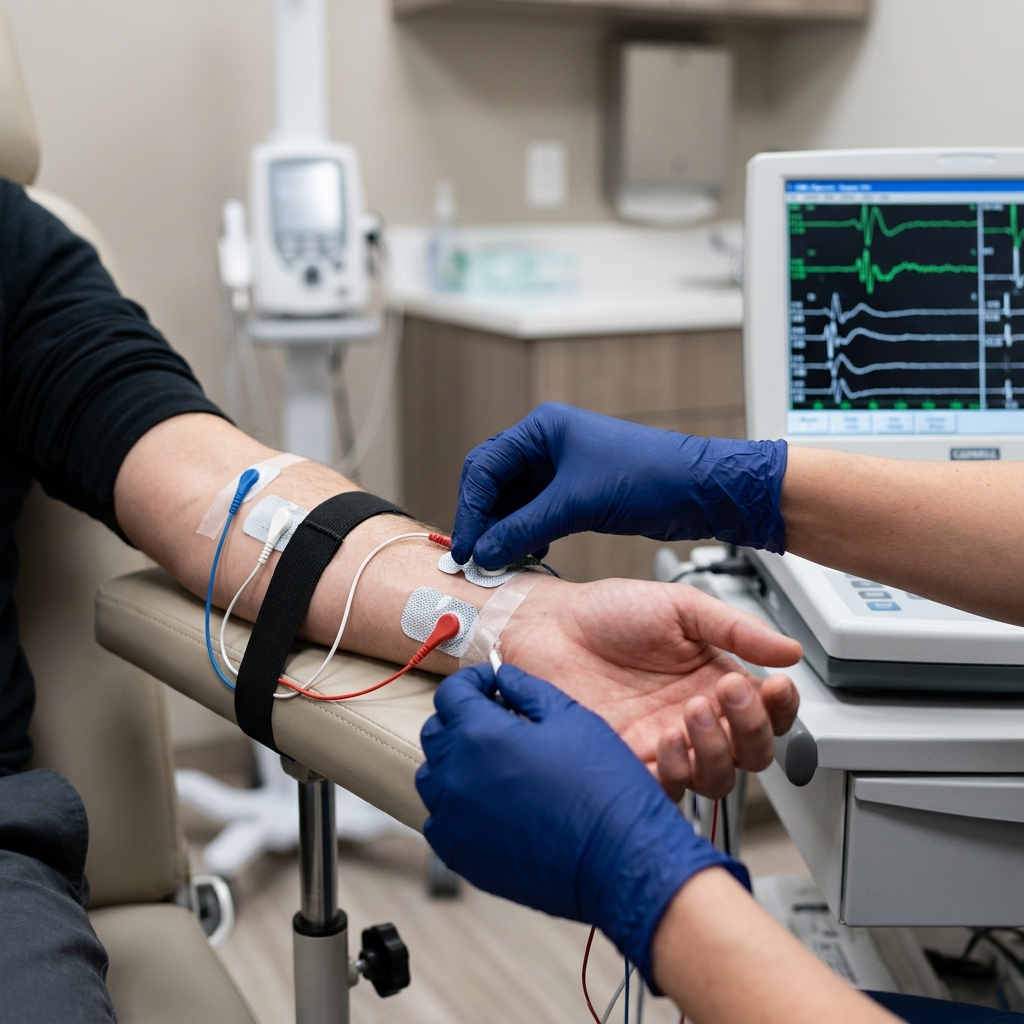
What is Precision EMG-NCV Diagnostic Testing?
When you experience shooting pain, muscle weakness, or a persistent 'pins and needles' sensation, the problem often originates deep within your nervous system. Standard physical exams and X-rays cannot see how your nerves are functioning. Precision Electromyography (EMG) and Nerve Conduction Velocity (NCV) testing are the clinical gold standards for evaluating the true physiological health of your peripheral nerves and muscles.
This diagnostic procedure is actually two separate, complementary tests. The NCV (Nerve Conduction Velocity) test utilizes mild electrical impulses applied to the skin to measure exactly how fast and how well your body's electrical signals are traveling along your nerve pathways. The EMG (Electromyography) portion involves inserting a microscopic, sterile pin directly into specific muscles to record their electrical activity, both at rest and during contraction. Together, these tests allow Dr. Rabara to map the exact location and severity of nerve compression, axonal damage, or demyelination.
What Conditions Does an EMG-NCV Diagnose?
Why Do I Need an EMG if I Already Had an MRI?
Many patients ask why they need nerve testing if they have already undergone an MRI. The answer lies in the difference between anatomy and function.
The MRI (The Picture)
An MRI is like taking a high-resolution photograph of the wires in a house. It can show if a wire (nerve) looks pinched by a wall (herniated disc). However, it cannot tell you if electricity is actually flowing through that wire.
The EMG-NCV (The Electricity Test)
Our testing acts as the electrician's multimeter. Even if a nerve looks slightly compressed on an MRI, the EMG-NCV provides the objective data to prove whether that compression is actually causing measurable electrical damage or disrupting the signal.
Is an EMG-NCV Diagnostic Right for You?
Early detection of nerve compression is critical. Prolonged nerve entrapment can lead to irreversible axonal damage and permanent muscle atrophy.
Clinical Indications
- You constantly drop objects or have lost grip strength.
- You wake up with numb, tingling, or "asleep" fingers/toes.
- Electric-like pain shooting down your arm or leg.
- Need objective proof before carpal tunnel or spine surgery.
Screening Precautions
- Active bleeding disorders or use of heavy blood thinners.
- Cardiac pacemakers or implanted defibrillators (inform Dr. Rabara).
- Active skin infections at the proposed needle insertion sites.
In-Depth Clinical Science
Explore the Clinical Science: Electrophysiological Mapping & Nerve Velocity
Nerve Conduction Velocity (NCV) testing is based on the biological principle of saltatory conduction. In healthy peripheral nerves, the myelin sheath acts as an insulator, allowing electrical impulses to 'jump' between nodes of Ranvier at speeds typically exceeding 50 meters per second in the upper limbs. When a nerve is compressed (as in Carpal Tunnel Syndrome) or damaged by metabolic factors (as in Diabetic Neuropathy), this velocity drops or the signal amplitude diminishes. We measure these exact velocities to determine the health of the myelin and the underlying axon, providing an objective numerical baseline of your nervous system's health.
The diagnostic power of an NCV test lies in its ability to differentiate between Neuropraxia (temporary 'stunning' of a nerve), Axonotmesis (damage to the nerve fiber itself), and Neurotmesis (complete nerve severing). By analyzing the morphology of the sensory and motor responses, Dr. Rabara can predict your recovery timeline and determine if surgical intervention is truly necessary or if conservative physiatric management is the safer, superior path.
Interpreting Muscle Potentials: Identifying Denervation & Reinnervation
The Electromyography (EMG) portion of the test evaluates the electrical 'chatter' inside the muscle itself. In a healthy state, a resting muscle is electrically silent. However, when a nerve has been damaged or severed, the muscle fibers it once controlled becomes unstable and begin to "fire" spontaneously. We record this as Fibrillation Potentials or Positive Sharp Waves. These are the objective clinical markers of active denervation.
Conversely, the EMG can also detect signs of healing. We look for **Polyphasic Motor Unit Action Potentials (MUAPs)**, which indicate that the nerve is successfully 're-branching' and making new connections with the muscle. This process, known as reinnervation, is the scientific proof that your rehabilitation plan is working at a cellular level. By monitoring these waveforms, Dr. Rabara can provide a definitive prognosis on whether a weakened muscle can and will regain its strength.
Clinical Precision: Localizing Radiculopathy vs. Peripheral Neuropathy
Many patients present with leg pain that is vaguely called "sciatica." However, the source could be a pinched nerve in the low back (Radiculopathy) or a generalized nerve issue caused by diabetes or toxins (Peripheral Neuropathy). The EMG-NCV is the only test that can definitive differentiate these two. By testing specific muscles and nerve segments (e.g., Tibial, Peroneal, and Sural nerves), we can "map" the exact location of the bottleneck. This prevents unnecessary procedures—like treating a hand for Carpal Tunnel when the real problem is a pinched nerve in the neck (Cervical Radiculopathy). Precision diagnostics ensure that your treatment is targeted at the root cause, not just the symptom.
The 3-Step Testing Process
The Nerve Conduction Study (NCV)
We place surface electrodes on your skin and deliver brief, mild electrical impulses to map nerve speed and signal strength.
The Electromyography (EMG)
A micro-needle electrode is gently inserted into specific muscles to record internal electrical activity and detect muscle denervation.
The Clinical Diagnosis
Dr. Rabara analyzes the complex waveforms immediately to provide you with a precise, actionable diagnosis of your nerve health.
Common Questions
Does the EMG-NCV test hurt?
We prioritize your clinical comfort, but it is important to set honest expectations. The NCV portion feels like mild, static electrical shocks. The EMG portion involves the insertion of a tiny, sterile needle. Most patients find the test completely tolerable and agree that the momentary discomfort is entirely worth acquiring an accurate diagnosis.
How do I prepare for my EMG-NCV appointment?
Take a shower the morning of your test to remove natural skin oils. Do not apply any lotions, creams, oils, or moisturizers to your arms or legs. Wear loose-fitting, comfortable clothing. Continue taking your normal medications unless instructed otherwise.
Are there any medical risks or contraindications?
EMG-NCV is exceptionally safe. However, you must inform Dr. Rabara if you have a cardiac pacemaker, implanted defibrillator, or deep brain stimulator. Additionally, disclose if you have a bleeding disorder or are taking prescription blood thinners.
How long does the diagnostic procedure take?
The duration depends on the complexity of your symptoms. A simple screen may take 30 to 45 minutes, while a comprehensive evaluation of multiple limbs can take between 60 to 90 minutes.
Can I return to work or drive after the test?
Yes. There is absolutely no downtime or sedation. You can immediately resume normal activities, return to work, and drive yourself home. You may experience minor, localized muscle soreness which resolves quickly.
Why is it important that a Physiatrist performs this test?
The accuracy of an EMG depends entirely on the physician's real-time skill in placing electrodes and interpreting complex waveforms. As a specialized Physiatrist, Dr. Rabara possesses the advanced training required to execute the test and interpret the data accurately.
What happens after I get my results?
Dr. Rabara will sit down with you to explain the results and orchestrate a personalized, non-surgical treatment plan—whether that involves specialized injections, targeted physical therapy, or bracing.