Rapid, Pinpoint Relief from Acute Pain and Inflammation.
Don't let severe joint or tendon pain stop your day. Our dynamic, ultrasound-guided steroid interventions are meticulously designed to drastically reduce localized inflammation and help manage daily pain rapidly.
Message Us to Book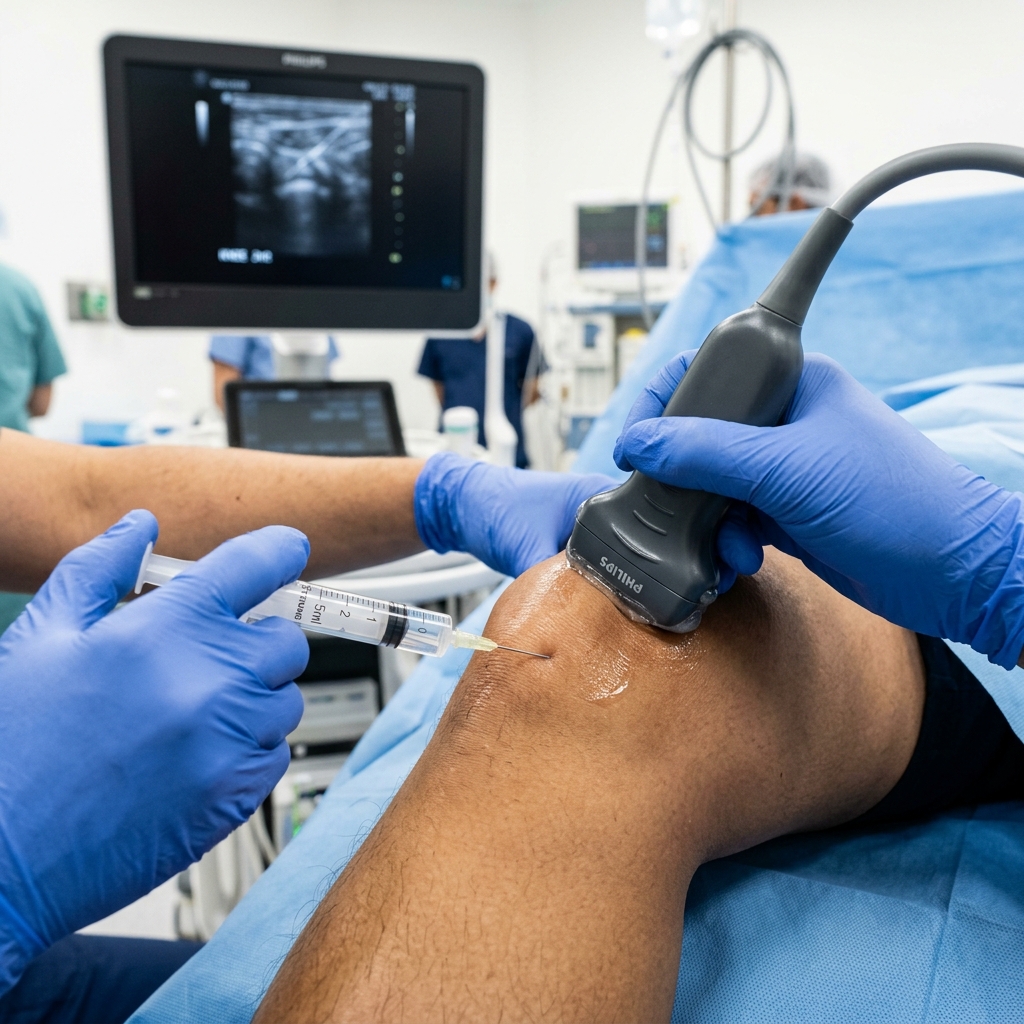
What are High-Precision Steroid Injections?
For patients suffering from acute flare-ups of arthritis, tendonitis, or bursitis, oral pain medications often prove insufficient, and resting for weeks is simply not an option. Corticosteroids are powerful anti-inflammatory agents that can be delivered directly to the specific anatomical site of your pain. This targeted approach results in much faster and more profound swelling reduction than systemic medication, allowing you to return to functional movement quickly.
The defining difference at TeraCare is our commitment to 100% Ultrasound Guidance. While many physicians still perform "blind" injections based on surface landmarks and feel, Dr. Rabara utilizes diagnostic MSK ultrasound to visualize the needle, the joint space, the tendon sheath, and the inflamed bursa in real-time. This eliminates guesswork, dramatically increases the anti-inflammatory medication's clinical efficacy, and ensures maximum patient safety by actively avoiding vital nerves or blood vessels.
What Conditions Respond to Steroid Injections?
Is a Guided Steroid Injection Right for You?
You are an EXCELLENT candidate if:
- You are experiencing an acute, severe pain flare-up that limits function or sleep.
- Oral NSAIDs or physical therapy have not provided sufficient relief.
- You require rapid management to facilitate your physical therapy protocol.
You may NOT be a candidate if:
- You have an active systemic or localized infection at the site.
- You have poorly controlled diabetes (can temporarily elevate blood sugar).
- Multiple injections have already been performed in the same joint this year.
The Realities and Rules of Corticosteroid Therapy
Corticosteriod injections are exceptionally safe when performed by a PARM-accredited physiatrist using ultrasound guidance. However, we prioritize informed clinical choice and complete risk transparency:
- Temporary Relief: A steroid injection is a powerful management tool, not a functional "cure." It drastically reduces inflammation to open a window of pain relief, which must be utilized for physical rehabilitation.
- Tissue Integrity: Repeated steroid injections (more than 3-4 per year in a single weight-bearing joint) can theoretically weaken tendon structure or accelerate cartilage degradation over the long term.
- Post-Injection Flare: While rare with ultrasound guidance, some patients experience a temporary increase in localized discomfort ('steroid flare') for 24-48 hours immediately following the procedure.
Steroid vs. Gel: Which Do You Need?
Powerful anti-inflammatory. It essentially 'extinguishes the fire' of active inflammation.
Mechanical lubricant and shock absorber. Think of it as 'greasing the hinges' of a creaky door.
The 3 Stages After Your Injection
The Local Anesthetic Phase
The injection often includes a localized numbing agent. You will feel immediate relief, which may wear off after several hours.
The Corticosteroid Active Phase
The actual steroid medication begins to reduce inflammation. You should notice progressive decreases in pain and morning stiffness.
The Rehabilitation Phase
Now that the pain is manageable, this is your critical window. We begin a customized physical therapy protocol to address the root cause.
Clinical Science & Technical Details
For our medical colleagues and highly analytical patients, we provide these transparent technical details on the pathophysiology and interventional protocols.
Explore the Clinical Science: How Guided Corticosteroids Defeat Inflammation
The physiological mechanism of intra-articular and periarticular corticosteroid injections is rooted in profound cellular suppression of the inflammatory cascade. When a patient in Vigan City presents with an acute musculoskeletal flare-up, their body is overproducing inflammatory cytokines, prostaglandins, and leukotrienes.
Medications like triamcinolone acetonide act by inhibiting phospholipase A2, thereby cutting off the arachidonic acid pathway. This essentially "starves" the inflammation at a molecular level, reducing capillary permeability and suppressing polymorphonuclear leukocyte migration.
Detailed Diagnostic Criteria & Targeted Anatomical Pathways
At TeraCare, recognize that no two inflammatory conditions are anatomically identical. For shoulder impingement and subacromial-subdeltoid bursitis, inflammation occurs within the tight confines of the coracoacromial arch. Guided injections allow us to navigate this space to bathe the bursa without puncturing the supraspinatus tendon.
In the wrist, conditions like Carpal Tunnel Syndrome require absolute sonographic mastery; the corticosteroid must be injected deep to the flexor retinaculum but superficial to the median nerve. Without ultrasound, this is a dangerous guessing game.
Inside the Treatment Room: Our Step-by-Step Sonographic Protocol
We adhere strictly to aseptic techniques, utilizing medical-grade chlorhexidine or povidone-iodine to sterilize the skin. The ultrasound transducer probe is encased in a sterile sheath. Dr. Rabara performs a "scout scan" to definitively map local neurovascular structures.
As the procedural needle is introduced, both you and the physician can watch its bright, hyperechoic reflection on the high-definition monitor. Visual confirmation is the ultimate guarantee of clinical precision, offering peace of mind that no blind injection could ever provide.
Pharmacokinetics & The Hybrid Treatment Pathway
Understanding the distinct pharmacokinetics of orthobiologic and pharmacological injections is vital. If a patient presents with a "hot," swollen, and highly inflamed knee, injecting gel directly into that hostile environment will often cause the HA molecules to degrade rapidly.
This is why Dr. Rabara often utilizes a phased, hybrid clinical pathway. Step one involves utilizing a high-precision steroid injection to rapidly extinguish the severe inflammatory cascade. Once the joint has chemically "cooled down," the environment is perfectly primed for Viscosupplementation or cellular Regenerative Medicine.
The 3-Step Clinical Process
Diagnostic Verification
We conduct a targeted clinical and ultrasound assessment to confirm active inflammation and ensure an injection is the appropriate clinical pathway.
Real-Time Guided Procedure
Utilizing high-resolution ultrasound, Dr. Rabara actively visualizes the needle trajectory to deliver the strong anti-inflammatory medication precisely into the inflamed target tissue.
Rapid Functional Milestone
Following the procedure, you will receive specific instructions to maximize the "window of relief" and begin structured, gentle physical rehabilitation.
Common Questions
Does a guided steroid injection hurt?
Patient comfort is paramount at TeraCare. While some anatomical structures are naturally sensitive, we utilize extremely fine, thin medical needles and administer a local numbing agent prior to the procedure. Most patients agreed that the momentary, tolerable discomfort of the injection is vastly outweighed by the profound and rapid relief.
How quickly will I feel relief, and how long does it last?
Every patient's physiological response is unique. Generally, significant pain relief begins within 48 to 72 hours as the anti-inflammatory cascade takes full effect. The duration of relief varies wildly by condition and severity, typically ranging from 6 weeks to 6 months.
Are there any side effects to the steroid medication?
Local corticosteroid injections are generally well-tolerated. Rare but possible localized side effects include skin depigmentation or fat atrophy at the injection site. Rare systemic effects may include facial flushing for 24-48 hours or a temporary, reversible elevation in blood sugar in diabetic patients.
Why must I have ultrasound guidance for my injection?
We believe that point-of-care ultrasound is the non-negotiable standard of care for modern medical interventional safety and clinical efficacy. "Blind" injections have been shown in medical literature to have failure rates up to 40% in certain joints because the medication never reaches the precise target.
Is this procedure covered by PhilHealth or do I pay cash?
We offer multiple accessible pathways for our patients. For specific, medically indicated conditions, Dr. Rabara can perform these high-precision steroid injections under PhilHealth sponsorship, significantly reducing or eliminating your out-of-pocket procedural costs.