Stop the Fall Before It Happens. Preserve Their Independence.
For a senior, a fall is never just a bruise—it is a life-altering event. Our physician-led geriatric physical therapy and balance programs rebuild strength, restore confidence, and keep your aging parents safe at home.
Message Us to Book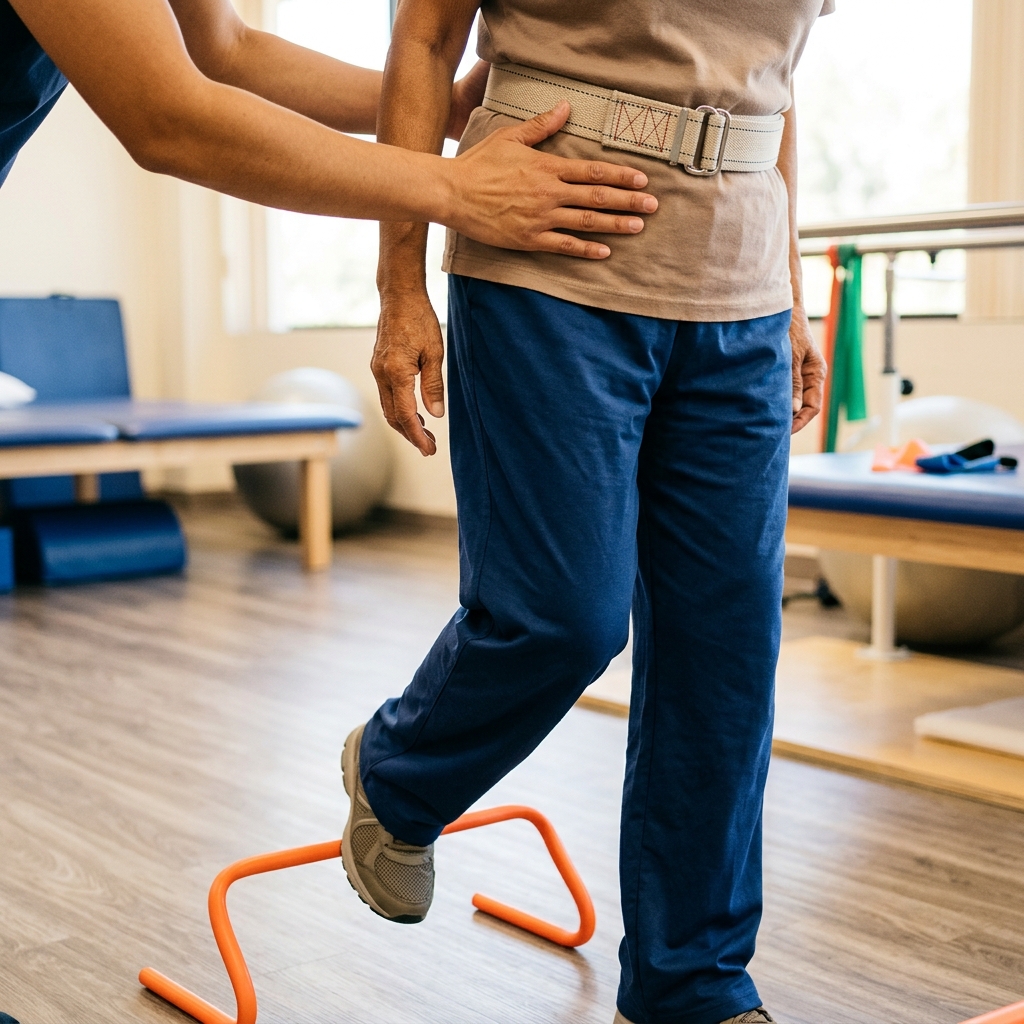
Protecting the Seniors We Love
As an adult child, watching your parents age is deeply stressful. You may have noticed them holding onto furniture to cross the living room, shuffling their feet to avoid tripping, or having "close calls" in the bathroom. You carry the constant dread of getting that phone call—the one saying they have fallen. For an elderly patient, a fall often leads to catastrophic fractures, lengthy hospitalizations, and a permanent loss of the dignity and independence they cherish.
Treating an aging body requires far more than generic exercise. Seniors frequently manage complex medical backgrounds, including hypertension, osteoporosis, and heart conditions. At TeraCare, safety is our highest mandate. As a medical doctor, Dr. Rabara rigorously screens your parent’s cardiovascular health, bone density, and current medications before a single exercise begins. We rebuild their balance safely, so you can stop worrying and they can start living confidently again.
Geriatric Conditions We Manage
Is Balance Therapy Right for Your Parent?
We understand that aging parents value their independence and often hide their struggles because they do not want to become a \"burden\" to their children.
Good Candidate If:
- "Furniture surfing" (grabbing walls/chairs to navigate the house).
- Suffered a recent slip, trip, or minor fall (even if uninjured).
- Severely weakened after recent hospital discharge and bed rest.
- Expressing a fear of leaving the house due to unsteadiness.
Not a Candidate If:
- Currently experiencing acute, unstable cardiac symptoms (chest pain).
- Completely bedbound/non-responsive without medical clearance.
- Unmanaged system instability prevents any safe mobilization.
The Realities of Senior Rehabilitation
Rebuilding an aging body is a delicate, gradual process. We prioritize slow, steady progress over aggressive, high-risk exercises. Here is what families need to know:
- Safety is Non-Negotiable: Your parent will never be left unattended. We utilize gait belts and parallel bars to guarantee they are 100% secure.
- Muscle Fatigue is Expected: Waking up dormant muscles causes fatigue. We differentiate between healthy fatigue and dangerous joint pain for comfort.
- Rebuilding Confidence Takes Time: The psychological fear of falling is just as debilitating as physical weakness. We celebrate small, functional victories.
Why Medical Geriatric Therapy is Different
Home Confinement
Mechanism: Encouraging sitting all day to avoid falling.
Drawbacks: Disastrous. Causes massive muscle wasting and stiff joints, making a severe fall inevitable when they do stand up.
Verdict: Extremely dangerous loss of independence.
Physiatrist-Led Senior Care
Mechanism: Dr. Rabara screens heart, bones, and medications. Therapists guide gentle, clinically secure balance protocols.
Drawbacks: Requires family support for consistent clinic visits.
Verdict: Safest way to restore dignity and mobility.
Generic Gyms or Standard PT
Mechanism: Using standard gym equipment or unspecialized routines.
Drawbacks: Does not account for fragile bones, complex heart medications, or unique neurological deficits.
Verdict: Lacks the required medical oversight for fragile seniors.
In-Depth Clinical Science
Explore the Clinical Science: Sarcopenia, Proprioception, and Polypharmacy
Physiological decline associated with aging is multi-system. Sarcopenia—loss of Type II fast-twitch muscle fibers—impairs the rapid postural reactions needed to catch a trip. Sensory degradation (Vestibular, Visual, Proprioceptive) delays data about spatial orientation. We also evaluate the dangers of Polypharmacy (anti-hypertensives, sedatives) which frequently induce orthostatic hypotension or CNS depression—massive pharmacological drivers of mechanical falls.
Detailed Diagnostic Pathways for Geriatric Syndromes
For Osteoporosis, we focus on axial extension and avoid loaded spinal flexion to prevent compression fractures, using CKC exercises to stimulate bone density. For Peripheral Neuropathy, we train visual and vestibular compensation. For Parkinson’s, we deploy high-amplitude neuromuscular strategies (LSVT BIG principles) to counteract gait freezing and bradykinesia.
Advanced Systemic Contraindications & Cardiac Safety
Safety is the foundation. We screen for acute cardiopulmonary instability (angina, symptomatic aortic stenosis) to prevent fatal events during exertion. For patients with cognitive decline (Dementia/Alzheimer's), we modify protocols using implicit motor learning and highly repetitive single-step cues to ensure compliance and safety.
Bone Density Integrity and Fracture Mitigation Protocols
Mechanical fragility means the margin for error is zero. Generic gyms risk devastating hip fractures. We utilize specialized perturbation training in a controlled environment, challenging limits of stability (ankle/hip/stepping strategies) without actual ground impact. We progress conservatively from static base support to dynamic dual-tasking scenarios.
Inside the Blueprint: Clinical Fall Risk Assessments
Foundation is metric-driven evaluation. We utilize globally validated scales: Timed Up and Go (TUG) for dynamic balance (>12s = high risk), Berg Balance Scale (BBS) for 14 functional tasks, and Tinetti POMA for gait and balance deficits. This data allows Dr. Rabara to track adaptation and definitively ensure interventions are lowering fall probability.
Neuromuscular Re-education and Reaction Time Adaptations
Aging nervous systems require consistent re-education. We induce neuroplastic changes in motor recruitment. Therapists focus on postural motor synergies: Ankle strategy (small sway), Hip strategy (larger sways), and Stepping strategy (massive center of gravity loss). If structural pain inhibits retraining, we may deploy ultrasound-guided injections to provide a comfortable functional window.
The Phases of Rebuilding Confidence
Assessment & Core Stability (Weeks 1-3)
Safety first. We begin with gentle, seated and supported exercises to wake up core and hip muscles without risk of a fall, focusing heavily on posture correction.
Dynamic Balance & Lower Body Strength (Weeks 3-6)
Building the "catch" muscles. Under strict supervision, we practice weight shifting and standing balance, training the legs to react quickly if they stumble.
Functional Independence (Weeks 6+)
Real-world navigation. We practice stepping over obstacles and navigating tight spaces safely to ensure they can stay independent in their own home.
Stop Worrying. Keep Them Safe and Independent.
The Safe Path to Independence
The Medical & Fall Risk Assessment
Dr. Rabara evaluates your parent's joint health, reflexes, and medication list. We conduct specific clinical balance tests to identify exactly why they are feeling unsteady.
The Balance & Strength Protocol
Using safety belts and parallel bars, our therapists gently guide your parent through exercises that strengthen the legs, improve posture, and retrain the brain's balance centers.
Home Safety & Independence
We teach your parent how to safely get out of bed, rise from a chair, and navigate stairs. We will also recommend the exact cane or walker they need, if necessary, to maximize their safety at home.
Common Questions
My parent is terrified of falling during therapy. Is it safe?
Absolute safety is our guarantee. Your parent will be constantly supervised by a trained physical therapist. We utilize clinical safety equipment, including heavy-duty gait belts and sturdy parallel bars, ensuring that a fall during their therapy session is virtually impossible.
Can therapy really help if my parent is already in their 80s or 90s?
Yes, absolutely. It is a medical myth that you cannot build muscle or improve balance in your 80s. While the process is gentler and more gradual, the elderly nervous system and musculature respond exceptionally well to targeted, consistent physical therapy.
Is Geriatric Physical Therapy covered by PhilHealth or HMOs?
Yes. Medically necessary physical therapy, particularly for patients recovering from prolonged hospitalization, severe weakness, or a recent stroke, is frequently eligible for coverage under PhilHealth and major HMO providers. We also proudly honor Senior Citizen and PWD discounts.
Why do we need to see Dr. Rabara instead of just going straight to a therapist?
Seniors have complex profiles. Dr. Rabara (Physiatrist) evaluates the "whole patient," reviewing blood pressure medications, checking for silent heart conditions, and assessing bone density to ensure therapy is medically safe for their internal health.
Do you help with prescribing canes, walkers, or wheelchairs?
Yes. Buying the wrong walking aid can actually increase fall risk. Dr. Rabara provides formal medical assessments to prescribe the exact assistive device your parent needs and trains them on how to use it properly and safely.