Safe Swallowing Assessments for Dysphagia and Feeding Tube Clearance.
Ensure your loved one can safely eat, drink, and communicate. We provide expert clinical swallowing evaluations to prevent complications and safely guide NGT or tracheostomy removal.
Message Us to Book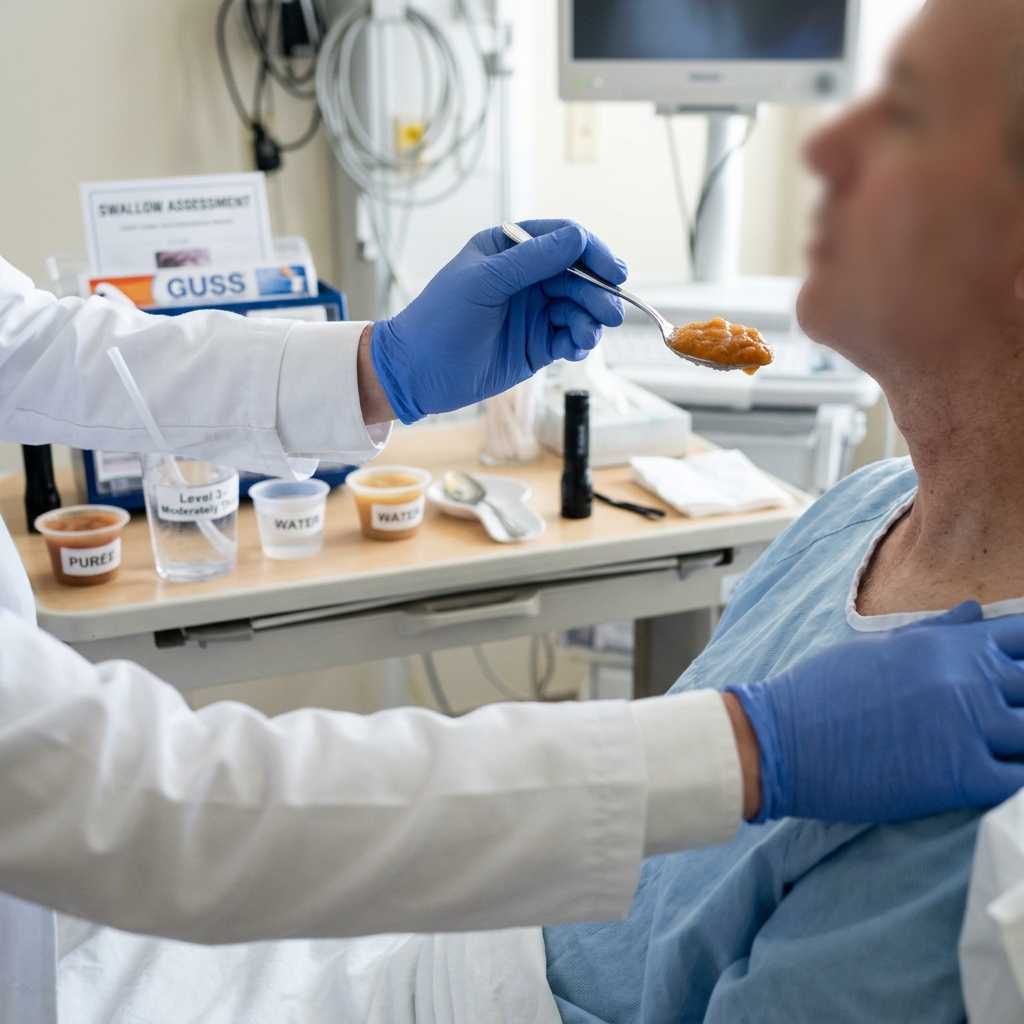
What is a Clinical Swallowing Assessment?
After a stroke, traumatic brain injury, or prolonged ICU intubation, the complex muscles required for swallowing often become weak or uncoordinated. This condition, called Dysphagia, carries a severe risk of aspiration—where food or liquid enters the lungs instead of the stomach, potentially causing life-threatening pneumonia.
To ensure patient safety, Dr. Rabara performs a functional clinical swallowing evaluation, utilizing protocols like the Gugging Swallowing Screen (GUSS). By carefully observing the patient's ability to process different textures—from pureed foods to thick liquids and regular water—we can objectively determine their exact swallowing capability without immediately requiring invasive equipment.
Who Requires a Swallowing Assessment?
Recognizing the Signs of Swallowing Impairment
Often, swallowing difficulties are not obvious. "Silent aspiration" can occur without outward choking, making a professional clinical evaluation absolutely critical for your loved one's safety.
Clinical Indications
- Frequent coughing or "gurgly" voice during or after meals.
- Current NGT or PEG tube dependence wishing to transition to oral eating.
- Tracheostomy tube in place requiring clearance for decannulation.
- Unexplained weight loss or recurrent respiratory infections.
Clinical Limitations
- Patient is medically unstable or unable to remain alert for evaluation.
- Suspected structural esophageal blockage (requires GI referral).
- Acute respiratory distress requiring immediate emergency intervention.
The Realities of Swallowing Recovery
Restoring a patient's ability to eat independently is our primary functional goal, but safety dictates our timeline.
In-Depth Clinical Science
Explore the Clinical Science: The Pathophysiology of Post-Stroke Dysphagia
The neuroanatomical coordination required for a safe swallow is one of the most complex tasks the human body performs, involving over 30 pairs of muscles and multiple cranial nerves. When a cerebrovascular accident (stroke) or traumatic brain injury occurs, the cortical control over these voluntary movements—and the brainstem's control over involuntary reflexes—is often disrupted. This leads to oropharyngeal dysphagia, where the patient cannot properly propel a food bolus or protect their airway. The scientific concern is not just choking, but "silent aspiration." In such cases, food or liquid enters the trachea and lungs without triggering a cough reflex, leading to aspiration pneumonia, which remains a leading cause of mortality in post-stroke patients globally and within the Philippines.
At TeraCare, we utilize evidence-based screening protocols, specifically the Gugging Swallowing Screen (GUSS), to objectively quantify this risk. Unlike traditional screens, the GUSS is a stepwise assessment that identifies exactly which texture is safe. By testing saliva, then semisolids, then liquids, we can prevent aspiration during the test itself. This clinical precision allows Dr. Rabara to make definitive, non-subjective recommendations for diet modification or the continued necessity of enteral feeding (NGT), ensuring that every step toward oral recovery is measured against the highest standards of neurological safety.
Advanced Indications: GUSS-ICU & Post-Extubation Protocols
Following prolonged mechanical ventilation in an Intensive Care Unit (ICU), patients often suffer from "post-extubation dysphagia." The physical presence of a tube can desensitize the laryngeal mucosa, while muscle disuse leads to rapid atrophy of the pharyngeal constrictors. In our Vigan City practice, we emphasize that even if a patient is awake and alert (Richmond Agitation-Sedation Scale 0 to -1), their swallowing reflexes may still be severely delayed. We monitor for clinical red flags such as a "wet voice" quality, reduced hyolaryngeal excursion, and delayed trigger of the swallow reflex. Identifying these deficits early allows us to implement sensory stimulation and compensatory strategies before the patient attempts to eat, preventing the devastating cycle of recurrent ICU readmission for pneumonia.
Detailed Anatomical Review: The 4 Stages of a Safe Swallow
To rehabilitate dysphagia, we must first isolate exactly which phase of the swallow is failing. Our comprehensive clinical assessment evaluates:
1. Oral Preparatory Phase: Coordination of the lips, tongue, and jaw to chew and form a cohesive bolus. Weakness here leads to food "pocketing" in the cheeks.
2. Oral Transport Phase: The tongue pushes the bolus toward the back of the throat. A delay here increases the risk of the bolus falling into the airway before the protective reflexes have triggered.
3. Pharyngeal Phase: The critical "point of no return" where the vocal cords close, the epiglottis tilts, and the bolus is diverted into the esophagus. This phase must happen in less than one second.
4. Esophageal Phase: The final transport into the stomach. While often managed by GI specialists, dysmotility here can cause "backup" and late-stage aspiration.
Neuromuscular Re-education: The Phased Rehabilitation Mandate
If our diagnostic evaluates identify significant impairment, we transition the patient into a specialized rehabilitation phase based on the principles of neuroplasticity. We don't just 'hope' the swallow returns; we actively train it. This includes Compensatory Techniques (such as the chin-tuck maneuver or supraglottic swallow to physically protect the airway), Sensory Stimulation (utilizing thermal or tactile input to wake up delayed reflexes), and Restorative Exercises (such as the Shaker maneuver or Masako exercise to physically strengthen the pharyngeal and laryngeal muscles). As a specialized physiatry clinic serving the Ilocos Region, we provide the medical oversight to ensure these exercises are performed safely without risking aspiration during therapy.
Your Diagnostic & Treatment Pathway
Moving Forward After the Assessment
Scenario A: Swallowing is Impaired
If our evaluation determines that swallowing remains unsafe, Dr. Rabara will prescribe a specific rehabilitation protocol. We coordinate closely with specialized Occupational Therapists (OT) or Speech-Language Pathologists (SLP) to rebuild swallowing strength through targeted exercises and diet modifications.
Scenario B: Swallowing is Safe
If the patient passes the functional assessments, Dr. Rabara will provide the formal medical clearance required to authorize the removal of their Nasogastric Tube (NGT) or recommend tracheostomy decannulation, allowing them to reclaim their dignity and oral independence.
The 3-Step Process
Clinical Bedside Evaluation
We conduct a thorough, step-by-step assessment of the patient's oral motor control and swallowing reflexes.
Diagnostic Coordination
If necessary, we seamlessly coordinate advanced endoscopic testing (FEES) with PhilHealth-accredited ENT specialists.
Targeted Action Plan
We issue a formal medical directive for either progressive therapy or safe apparatus removal.
Common Questions
Does the clinical swallowing assessment hurt?
Not at all. The functional clinical assessment (like the GUSS protocol) is completely non-invasive. It involves observing the patient while they attempt to swallow different textures, starting with mere drops of water or pureed food, to ensure their utmost safety and comfort.
Will Dr. Rabara remove the NGT or Tracheostomy during this visit?
Dr. Rabara performs the critical evaluation and provides the formal medical clearance needed for removal. Depending on the specific apparatus and the patient's primary care team, the actual physical removal may be coordinated with their attending physician, surgeon, or nursing staff based on our definitive recommendation.
What is a FEES test, and why might we need it?
FEES stands for Flexible Endoscopic Evaluation of Swallowing. If our initial bedside screen indicates 'silent aspiration' (choking without coughing), we may refer you for a FEES. An ENT specialist will pass a tiny camera through the nose to directly view the throat during a swallow, providing absolute diagnostic certainty.
Is the FEES test covered by PhilHealth?
If Dr. Rabara determines that an instrumental FEES test is medically necessary, we strategically refer our patients to affiliated ENT specialists who can often perform this procedure under PhilHealth coverage, helping alleviate the financial burden on your family.